Emergency Dentistry
Root Canal Recovery, Pain, and Visit Count: What Spring Patients Actually Need to Know
Reviewed by Dr. Ali Tameemi, DDS
Most patients recover from a root canal within a few days, and modern anesthesia makes the procedure far less painful than its reputation suggests. How many visits you need depends heavily on which tooth is being treated and how severe the infection is.
Why Your Tooth Type Changes Everything About the Procedure
One detail many patients don't realize until they're in the treatment chair: a root canal on a front tooth and a root canal on a back molar are genuinely different procedures in terms of time, complexity, and recovery. For Spring-area patients experiencing severe tooth pain, a dental emergency evaluation can help determine whether an endodontic procedure is the right next step.
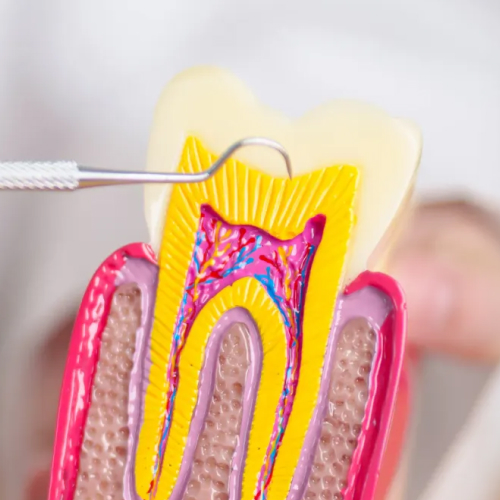
Front teeth (incisors and canines) typically have a single canal. In straightforward cases, the entire procedure can often be completed in one appointment lasting under 90 minutes. Back molars, by contrast, commonly have three or four canals — and in older patients, those canals can become calcified and narrow, requiring more careful navigation. That's the primary reason some patients need two visits while others don't.
There's another physical reality that rarely gets mentioned: jaw fatigue. When a patient is holding their mouth open for 90 minutes or more on a complex molar case, the muscles around the jaw get tired. That soreness after a multi-canal procedure often isn't from the nerve treatment itself — it's from the prolonged positioning. As the American Association of Endodontists explains, modern root canal treatment is very similar to a routine filling, but the time required varies by case complexity.
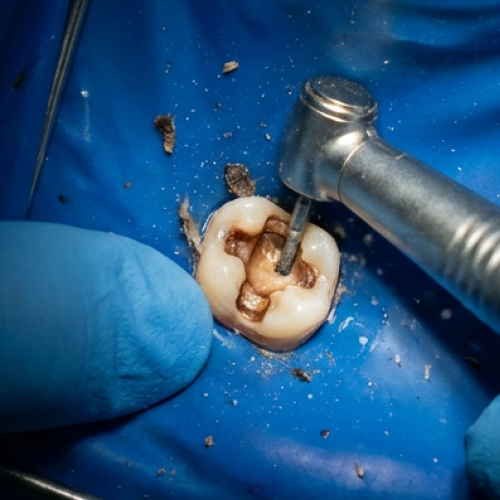
For multi-visit cases, the first appointment handles cleaning and disinfection. A temporary filling seals the tooth between visits. During that 7–14 day window, the tooth may feel more sensitive around day three than it did right after the appointment. That's usually the antimicrobial medication working inside the canal — not a sign something went wrong. Running the tongue across the temporary filling daily can help monitor it. It should feel slightly raised but smooth. If it feels sunken or hollow, the dental office should be contacted promptly. A compromised temporary seal is the main risk during the inter-appointment period, because bacteria from saliva can re-enter the canal. Avoid chewing on that side entirely — not just hard foods, but anything that puts direct biting pressure on the tooth before the permanent crown is placed.
What You'll Actually Feel During the Procedure
The fear around root canals almost always comes down to one question: will it hurt? The honest answer is that sharp, electric pain should be zero — that's what the local anesthetic is there to prevent. But patients frequently feel other sensations mid-procedure and panic, assuming the anesthesia has failed. Understanding what's normal helps enormously.
Here's a sensory breakdown of what's typical:
- Mechanical pressure: You'll feel the instruments working. This is not pain — it's vibration and pressure transmitted through your jaw and surrounding bone. It's completely normal.
- Vibration from rotary files: The instruments used to shape the canals create a mild buzzing sensation. Some patients describe it as similar to an electric toothbrush.
- The smell of disinfectant: The canals are irrigated with sodium hypochlorite. You may notice a faint bleach-like smell. This is expected and harmless.
- Pressure during filling: When the canal is sealed with gutta-percha, you may feel brief pressure. Again, not pain.
If at any point a sharp or shooting sensation occurs, raising a hand signals the clinician to add more anesthetic. Research published in PMC confirms that supplemental anesthesia techniques are available when standard injections need reinforcement — particularly for mandibular teeth, which are statistically harder to numb fully.
According to Cleveland Clinic, most patients report that a root canal is no more painful than getting a filling. The pain people associate with the procedure is usually the pre-treatment infection, not the treatment itself.
How Long Recovery Actually Takes
For most patients, meaningful recovery happens within three to five days. There will likely be some tenderness when biting down and mild sensitivity for the first 48–72 hours. Over-the-counter ibuprofen handles this well for the majority of people.
A few things influence how quickly recovery progresses:
Severity of the infection before treatment. Teeth that were already acutely painful tend to have more post-procedure soreness. The surrounding tissue has been inflamed, and it takes time to settle even after the source of infection is removed. Untreated gum disease and gingivitis can compound this inflammation and slow the healing process.
Which tooth was treated. As noted earlier, molars with multiple canals require more instrumentation time. More instrumentation means slightly more post-operative sensitivity — though this typically resolves within the same general timeframe.
Whether the crown is placed promptly. This is critical and often underestimated. Research from Healthline notes that pain after a root canal should decrease steadily over time. But a tooth without its permanent tooth crown is structurally vulnerable. Delaying the crown appointment isn't just inconvenient — it puts the tooth at risk for vertical fracture, which can make the tooth unrestorable.
According to the Mayo Clinic, root canal treatment is designed to save a damaged tooth rather than remove it. A properly treated and restored tooth can function for decades. The key word is restored — the crown is part of the treatment, not optional follow-up.
Contact the dental office if swelling worsens after day two, pain increases rather than decreases, or a temporary filling has shifted or come out completely.
How Many Visits Will You Need?
For most straightforward cases — a single-canal tooth with a contained infection — one visit is entirely realistic. For molars, teeth with severe infection, or cases where the anatomy is complex, two visits produce better outcomes because the inter-appointment period allows the antimicrobial dressing to work before final sealing.
Harvard Health notes that some dentists prescribe antibiotics before the procedure when the infection is severe, because a very inflamed tooth is harder to anesthetize fully. Visit count is ultimately a clinical decision made after examining X-rays and assessing the individual tooth — not a one-size answer.
After the root canal itself, plan for two additional appointments: one to prepare for the crown and one to place it. That sequence — endodontic root canal, temporary, crown prep, final crown — is the complete arc of treatment. Skipping any part of it affects long-term outcomes. In cases where the tooth cannot be saved, a tooth extraction followed by a restorative option such as dental implants may be the recommended path forward.
Schedule Your Consultation in Spring
For patients who have been putting off treatment because they're unsure what to expect, coming in for an evaluation is a helpful first step. At Nu Dentistry Spring, private suites and high-tech diagnostic tools are used to make the entire process as comfortable as possible for Spring, Texas patients. Understanding the specific tooth anatomy before treatment means fewer surprises and a clearer recovery plan. Staying current with cleaning and exam appointments is also recommended, as routine checkups are one of the best ways to catch issues before they require more complex treatment.
Medical disclaimer: This article is for informational purposes only and does not constitute professional medical or dental advice. Always consult a licensed dental provider regarding your individual oral health needs.